If you're taking blood pressure medication but your numbers still aren't where they should be, you're not alone. More than 80% of older adults in the United States aren't meeting dietary magnesium recommendations, and here in Memphis and Germantown, we're seeing the cardiovascular consequences play out in exam rooms every single day.
The issue isn't just about eating more leafy greens. It's about understanding why magnesium has become the most overlooked mineral in modern cardiovascular care: and why the standard blood test your doctor ordered probably missed your deficiency entirely.
Why Magnesium is the "Master Mineral" for Heart Health
Magnesium functions as a cofactor in over 300 enzymatic reactions throughout your body. That means without adequate magnesium, hundreds of critical processes simply can't happen efficiently: including the ones that keep your heart beating steadily and your blood vessels relaxed.
Here's what magnesium does for your cardiovascular system:
- Regulates heart rhythm and electrical conduction
- Relaxes blood vessel walls to lower blood pressure naturally
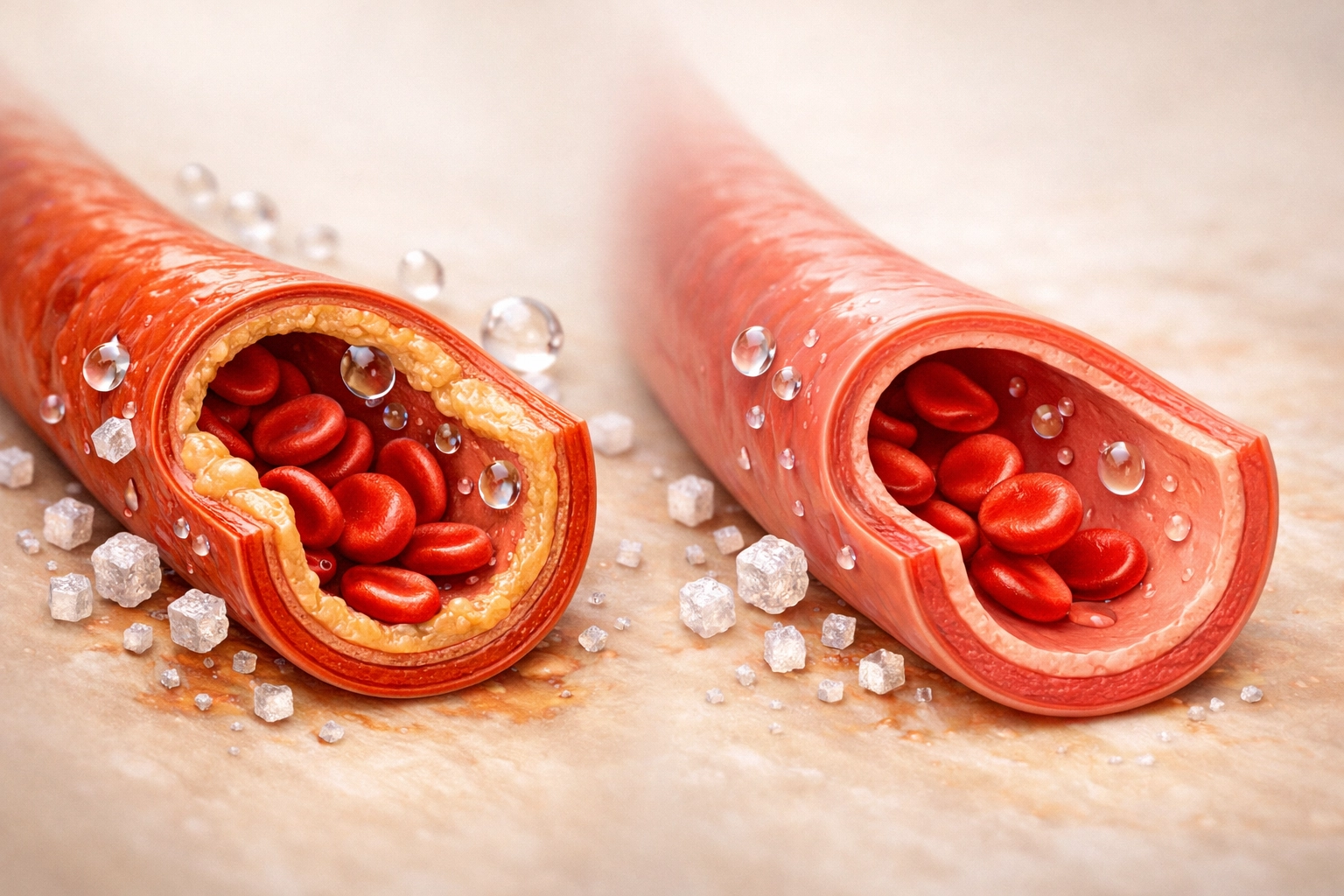
- Prevents calcium from building up in arterial walls
- Reduces inflammatory markers like C-reactive protein and interleukin-6
- Supports energy production in heart muscle cells
- Balances sodium and potassium for proper fluid regulation
When magnesium levels drop, your blood vessels constrict, inflammation increases, and your heart has to work harder to pump blood through tighter arteries. This is why magnesium deficiency is directly linked to hypertension, arrhythmias, and increased heart failure risk.

The Memphis Diet Problem: Why We're Setting Ourselves Up for Deficiency
Let's talk about why patients in Memphis, Germantown, Collierville, and Arlington face particular magnesium challenges. The traditional Southern diet: while delicious: is notably low in magnesium-rich foods and high in processed ingredients that actively deplete your body's magnesium stores.
The Standard Memphis Plate:
- Fried foods (cooked in oils that lack magnesium)
- White bread and refined grains (processing removes 80-90% of magnesium)
- Sweet tea and sodas (high sugar intake increases magnesium excretion)
- Limited dark leafy greens and nuts
- Heavy reliance on processed and packaged foods
Add to this the soil depletion problem. Modern agricultural practices have stripped minerals from farmland across the Mid-South. Even when you're eating vegetables, they contain significantly less magnesium than the same foods contained 50 years ago.
The result? Research shows approximately 75% of postmenopausal women consume less than the Recommended Daily Allowance for magnesium. The numbers are likely similar for men, though they're studied less frequently.
The Blood Pressure Connection: How Magnesium Lowers Your Numbers
Magnesium acts as a natural calcium channel blocker: the same mechanism used by prescription blood pressure medications like amlodipine. When you have adequate magnesium, it prevents excessive calcium from entering your heart and blood vessel cells, keeping them relaxed and flexible.
Low magnesium levels trigger a cascade of problems:
- Blood vessels constrict and stiffen
- Inflammatory markers rise (hs-CRP and IL-6 increase)
- Endothelial dysfunction develops (the inner lining of blood vessels stops working properly)
- Arterial walls become more prone to plaque buildup
- Heart rhythm irregularities become more common
Studies demonstrate that dietary magnesium intake is inversely associated with hypertension. In plain language: the less magnesium you consume, the higher your blood pressure tends to run.
For our patients in Memphis dealing with resistant hypertension: blood pressure that won't respond to medications: magnesium deficiency is frequently part of the picture. Correcting the deficiency often allows blood pressure medications to work more effectively, or reduces the number of medications needed entirely.

Why Your Doctor's Magnesium Test is Probably Wrong
Here's where things get frustrating. Most doctors order a Serum Magnesium test, which measures magnesium levels in your blood plasma. This test misses the majority of deficiencies because only 1% of your body's magnesium is in your bloodstream.
Your body tightly regulates serum magnesium levels because they're critical for heart function. When magnesium drops, your body pulls it from your bones, muscles, and tissues to keep blood levels stable. By the time a serum magnesium test shows low, you're severely depleted.
The better test: RBC Magnesium (Red Blood Cell Magnesium)
This test measures magnesium inside your cells: where 99% of your body's magnesium actually lives. It provides a far more accurate picture of your true magnesium status.
At The Fatigue Clinic in Collierville, we routinely see patients with "normal" serum magnesium but significantly low RBC magnesium levels. These are the patients walking around with undiagnosed deficiency, wondering why their blood pressure won't budge despite multiple medications.
Southern Soil and Water: The Local Magnesium Depletion Factor
The Memphis area sits on unique geology: we're dealing with depleted topsoil from intensive cotton farming that lasted more than a century. Modern agriculture focuses on nitrogen, phosphorus, and potassium, largely ignoring trace minerals like magnesium.
Additionally, our municipal water supply varies significantly in mineral content. While Memphis draws from a relatively pure aquifer, most water treatment processes don't add back minerals. If you're drinking filtered or bottled water (removing even more minerals), you're missing out on what used to be a reliable magnesium source.
Compare this to regions with mineral-rich soil and hard water: populations there naturally consume more magnesium through food and water, and cardiovascular disease rates tend to run lower.

Signs You Might Be Magnesium Deficient
Common symptoms include:
- Muscle cramps, especially at night
- Persistent fatigue despite adequate sleep
- Heart palpitations or irregular heartbeat
- High blood pressure that resists medication
- Anxiety and difficulty managing stress
- Headaches or migraines
- Difficulty sleeping or restless legs
- Constipation
Many of our patients from Germantown and Arlington come in assuming they need more potassium for their muscle cramps: but magnesium deficiency is often the real culprit.
What To Do About It: Testing and Treatment at The Fatigue Clinic
If you're dealing with high blood pressure, heart palpitations, or any of the symptoms above, the first step is proper testing. We use RBC Magnesium testing to get an accurate baseline, then create a personalized supplementation plan.
Magnesium supplementation isn't one-size-fits-all. Different forms of magnesium serve different purposes:
- Magnesium glycinate: Best absorbed, gentle on digestion, ideal for deficiency correction
- Magnesium taurate: Specifically supports cardiovascular function
- Magnesium threonate: Crosses the blood-brain barrier for neurological benefits
- Magnesium oxide: Poorly absorbed, acts more as a laxative
We also offer IV magnesium therapy for patients with severe deficiency or absorption issues. IV administration bypasses the digestive system entirely, delivering magnesium directly to your cells.
Don't Forget Your Heart's Bigger Picture: The $75 Cardiac Calcium Score
While you're addressing magnesium deficiency, it's the perfect time to get baseline information about your cardiovascular risk. We're currently offering Cardiac Calcium Scoring for just $75: a fraction of what hospitals charge.
This simple, non-invasive CT scan measures calcium deposits in your coronary arteries, giving you a precise picture of your heart disease risk. Combined with magnesium optimization, you're taking real, measurable steps to protect your heart health.
The calcium score is particularly valuable if you:
- Have family history of heart disease
- Have high blood pressure or cholesterol
- Are over 40 with cardiovascular risk factors
- Want to know if your current prevention strategy is working
Taking Action in Memphis and Germantown
Here at The Fatigue Clinic in Collierville, serving patients throughout Memphis, Germantown, and Arlington, we see magnesium deficiency affect cardiovascular health every single week. The good news? It's one of the most straightforward deficiencies to correct when properly identified and treated.
Ready to get your magnesium levels checked with the right test? Call us at 901-221-8621 to schedule comprehensive cardiovascular testing, including RBC Magnesium and our $75 Cardiac Calcium Score special.
Your blood pressure: and your heart( will thank you.)